Treatment for patients with breast cancer has come a long way since the first written descriptions of breast tumors more than 1,800 years ago. Humanity waited until the 17th century, when we began to understand the role of our circulatory system, to find a connection between breast cancer and the lymph nodes.
This essential finding led to procedures to remove lymph nodes, breast tissue and underlying chest muscles (a radical mastectomy) — the first evidence-based treatment option to treat breast tumors. William Halsted, M.D. performed the first radical mastectomy in 1882.
Patients with suspicious masses in their breasts were placed under anesthesia. If the tumor biopsy confirmed a breast cancer diagnosis, an immediate radical mastectomy was completed. Many women woke up only to be informed they had lost their entire breast – there was not a conversation between a doctor and the patient about treatment options. This remained the standard treatment until the mid-1970’s.
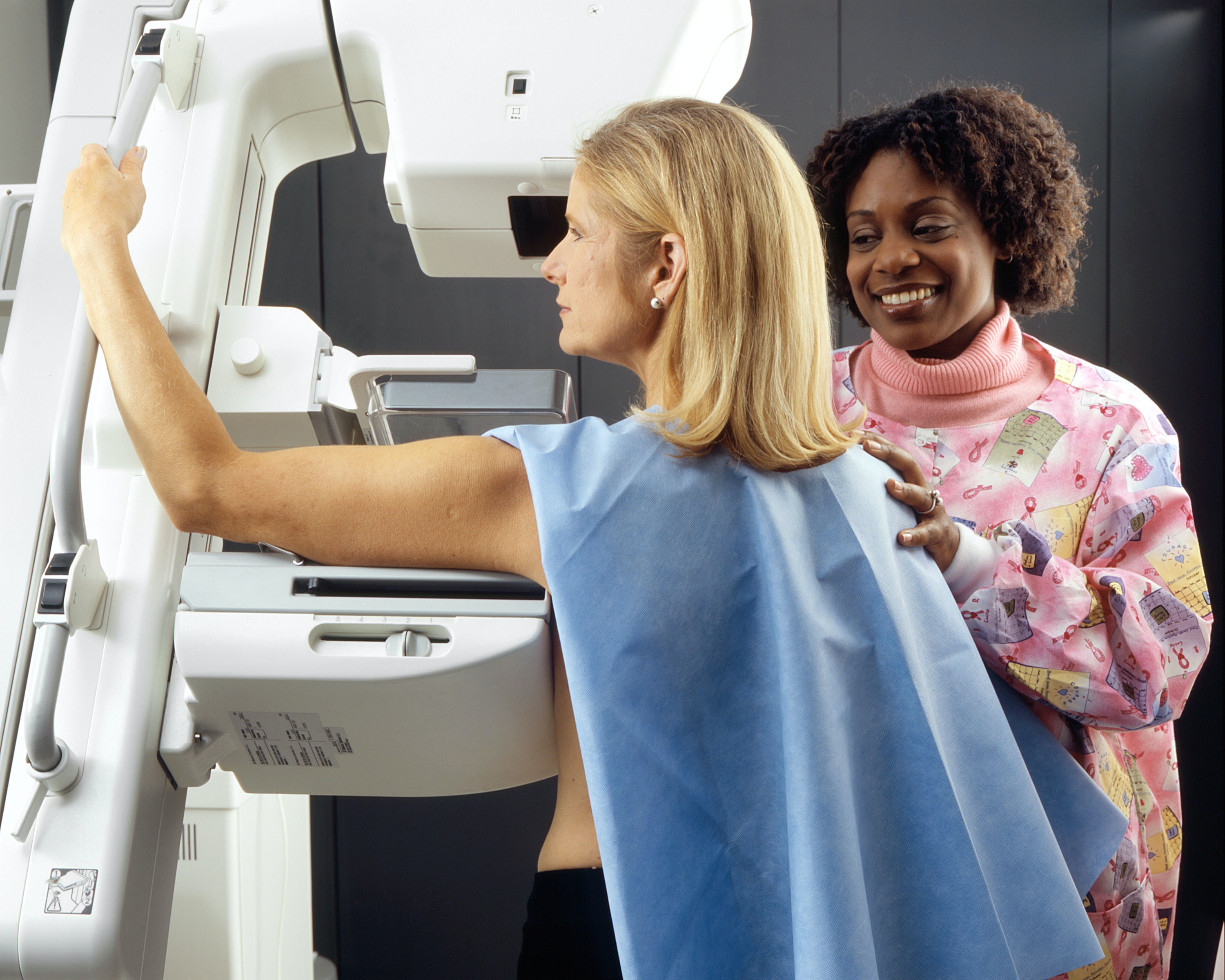
The invention of the modern mammogram in 1969 enabled doctors and patients to find smaller breast cancers. While x-rays had been in use for decades to detect breast cancer, it was not until this procedure could capture the image on film was early detection possible.
Finding smaller, usually more localized breast cancer spurred many doctors to experiment in less extensive breast surgery than the radical mastectomy. Controversially – at the time – some doctors started to practice a two-step approach to breast cancer treatment: 1) biopsy to confirm a diagnosis and 2) confer with patient before starting a treatment regime. This soon led to a substantial change in breast cancer treatment and patient participation.
In June 1974, Rose Kushner, a 45-year-old journalist, felt an “elevation” in her left breast. Kushner struggled to find a doctor who would only perform a biopsy – most doctors refused to separate a biopsy from an immediate radical mastectomy. Her family surgeon finally relented and confirmed a breast cancer diagnosis.
After researching breast cancer treatment options, Kushner decided she preferred a less invasive procedure than a radical mastectomy. Unable to find a surgeon near her home in Maryland, she traveled to Buffalo, NY where Dr. Thomas Dao performed a modified, less invasive, mastectomy (lumpectomy).
Using her journalist skills, Kushner became a tireless advocate for breast cancer. In just seven weeks Kushner wrote Breast Cancer: A Personal History and Investigative Report, which challenged an often times paternalistic medical culture in America. Kushner asserted every woman should know three things.
- The 1-step radical mastectomy was not current with medical knowledge.
- Cancer specialists provided superior care to general surgeons.
- Women must educate themselves about their disease, participate in the decision-making process and not be fearful of challenging their doctors.
These were radical notions in 1975. By 1979 the National Institutes of Health (NIH), in a conference on breast cancer, concluded the radical mastectomy was no longer appropriate for every breast cancer diagnosis. Kushner pushed the panel to go further and to reject the 1-step procedure – enabling women to make informed decisions about their treatment plan.
The same time period also saw conclusive, evidence-based studies that proved adjuvant systemic therapy (chemotherapy, hormonal therapy, radiation therapy) increased survival. The combination of early detection, additional treatment options and the fierce determination of patient advocates like Rose Kushner provided breast cancer patients more information to make choices.
This led to multi-disciplinary teams (oncologists, pathologists, radiation oncologists, radiologists and surgeons) participating in breast cancer treatment plans. The first freestanding center to combine different breast cancer specialists in one practice was the Van Nuys Breast Center (VNBC), founded in 1979 by Melvin Silverstein, M.D.
In a few short years breast cancer diagnosis and treatment had changed radically from a one-physician surgical disease to a much more complex disease that required a multidisciplinary team. — Breastlink founder John Link, M.D.



Add new comment